United Arab Emirates and WHO sign US$ 25 million cooperation agreement for Al Makassed Hospital in East Jerusalem

Under the directives of His Highness Sheikh Mohamed bin Zayed Al Nahyan, President of the United Arab Emirates, the country signed a US$ 25 million cooperation agreement in support of Al Makassed Hospital in East Jerusalem. This came as part of the United Arab Emirates’ efforts to support the medical and health care sectors in the occupied Palestinian teritory in collaboration with the World Health Organization (WHO) and in coordination with the Office of the United Nations Special Coordinator for the Middle East Peace Process (UNSCO).
HE Sultan Mohammed Al Shamsi, Assistant Minister of Foreign Affairs and International Cooperation for International Development Affairs, said that the signing of this agreement reflected the United Arab Emirates' consistent and historic commitment to the Palestinian people in meeting their humanitarian needs, especially in the health sector. The Assistant Minister highlighted the notable efforts of WHO and UNSCO in collaborating with the United Arab Emirates to strengthen the capacities of Palestinian hospitals in providing health care to the Palestinian people. At Al Makassed Hospital in particular, it is expected that more than 130,000 people will benefit from its health services.
“The COVID-19 pandemic has demonstrated that health is not a luxury, but a human right, and it is central to development,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. “We thank the United Arab Emirates for its generous donation, leading role and commitment to improving the delivery of quality health services for the Palestinian people.”
Lynn Hastings, United Nations Resident Coordinator for the Occupied Palestinian Territory, thanked the Government of the United Arab Emirates for its timely and generous support, which she said will help ensure the continuity of essential health services by Al Makassed Hospital, which is an important part of the East Jerusalem Hospital Network.
“The United Arab Emirates’ contributions will be vital in sustaining the immediate and critical delivery of essential health care services at Al Makassed Hospital, including referral cases,” said Dr Rik Peeperkorn, WHO Representative in the occupied Palestinian territory. “It will also improve the quality of Al Makassed’s Obstetrics and Gynecology Department and assist in the training of medical specialists for all of Palestine.”
Dr Adnan Farhoud, Director-General of Al Makassed Hospital, thanked President H.H. Sheikh Mohamed bin Zayed Al Nahyan for the humanitarian gesture and underscored the degree to which such support will transform the hospital’s operations and services.
Amal, 38, misses two appointments in three months for brain catheterization and scan

Amal, a 38-year-old woman from Gaza, was found to have a brain aneurysm (the potentially life-threatening ballooning of a blood vessel) in March 2022.
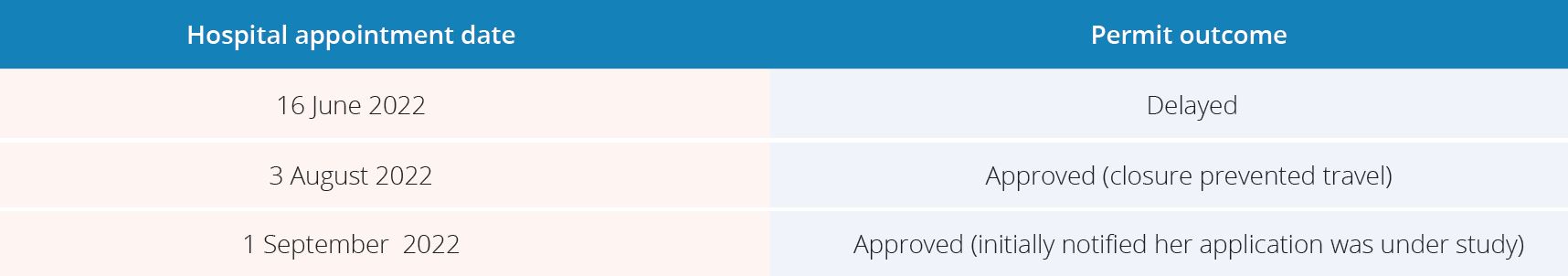
On 5 June 2022, Amal was referred to An-Najah University Hospital in Nablus, in the West Bank, for brain catheterization and scan (angiography), a procedure not available in the Gaza Strip. She made one permit application for an appointment on 16 June that was delayed. Amal was approved a permit to travel on 3 August but following closure of Erez (Beit Hanoun) checkpoint by Israeli authorities on 2 August she was unable to exit the Gaza Strip to receive care.
Talking about the outcome of her first application, Amal said, “I don’t know why I am prevented, I have been waiting so long! I need to have this test so the doctor can make a clear diagnosis and give me proper treatment. I suffer and worry every day.
”Amal received a further hospital appointment at An-Najah University Hospital for 1 September. She was eagerly awaiting a text message from the Palestinian Health Liaison Office, hoping for a positive response, when WHO spoke with her the day before her appointment. She received the text at 5pm that day and called to ask, “I’ve just received a text message from the Liaison Office. It says under study. What does it mean?” After her initial disappointment, she received another message later that evening saying that she had been approved and could travel the next day.
Amal finally travelled and received the scan she needed. Doctors advised the best course of action would be to manage her condition with medicines, which she now takes daily. “I finally had the tests and I feel so grateful that I won’t need brain surgery after all. The doctors at An-Najah reassured me and prescribed me some medicines. They recommended that I will need follow up to keep an eye on things,” Amal said.
Ahmad’s journey to health
 26 September 2022 – It is playtime for Ahmad and his grandson as they enjoy playing football at a pitch in the Gaza Strip. They come here regularly for football and exercise. But just a few years ago, Ahmad’s life looked very different. Hospital visits instead of football with his grandson occupied most of his time.
26 September 2022 – It is playtime for Ahmad and his grandson as they enjoy playing football at a pitch in the Gaza Strip. They come here regularly for football and exercise. But just a few years ago, Ahmad’s life looked very different. Hospital visits instead of football with his grandson occupied most of his time.
In September 2019, Ahmad slipped on the stairs in his home. He suffered a major injury, which left him in pain for years. His family rushed him to the Abu Yousif Al Najar Hospital in Rafah city, where he was diagnosed with a complex fracture in his right leg.
“I had to undergo immediate surgery. Doctors told me that the recovery process would be long and painful, but none of us expected the pain and discomfort to last for what seemed like an eternity,” he says.
Ahmad, who’s been working as a senior nurse for the past 33 years, was forced to take a break from work due to persistent pain and limited mobility. He had to rely on crutches to move around and lived with severe pain for 18 months.
“I was in so much pain and agony, not just physically but also mentally. I wasn’t used to being dependent on anyone. I would always be helping others. After the accident, my life felt compromised. It was very distressing. I just wanted my normal life back,” he recalls.
After numerous visits to multiple doctors yielded no results, Ahmad was advised to seek assistance at the Limb Reconstruction Centre at the Nasser Medical Complex in the Gaza Strip.
Established by the Ministry of Health and WHO in November 2019, with support from the Swiss Development Cooperation, European Union Humanitarian Aid, the Foreign, Commonwealth and Development Office and the United Nations Office for the Coordination of Humanitarian Affairs, the Centre is the only medical centre in the Gaza Strip that offers high-quality all-inclusive treatment from initial care to surgery to rehabilitation, for patients with complex limb injuries. Thanks to support from donors, WHO has trained surgeons, physiotherapists and psychosocial support staff to introduce a multidisciplinary, patient-centred approach and provided equipment and supplies to ensure that the Centre can continue providing the highest level of care to patients.
Ahmad visited the Centre in February 2021 and finally got a diagnosis for his pain. He was suffering from a complicated non-healing fracture, which required major surgery.
“I felt hope once again. I had a shot at getting my leg and my life back,” says Ahmad.
He underwent urgent surgery and stayed at the centre for almost a month, where he received specialized care, including psychological support, physiotherapy, health awareness and tailored meals to aid his recovery. Within 6 months of being discharged, he gained full mobility and no longer needed to rely on his crutches to walk.
In the Gaza Strip, where escalating and reoccurring violence and limited access to outside specialized health care creates a huge burden on the fragile health system, the Limb Reconstruction Centre is helping to provide a new lease on life for patients by preventing disabilities and amputations and also restoring dignity and hope.
“It’s wonderful to have such services here as for most people leaving Gaza is just not an option. Preventing disability and helping people return to normal life has an even more profound impact in a place like this where people are already living under difficult circumstances,” says Ahmad.
Today, Ahmad is back at work doing what he loves the most – helping others and can still be found on the football field in the evenings with his grandchild. He is living life to the fullest and keeping active.

Keeping hope alive
 Aseel stands at the door of her office to welcome patients as they walk in. The entrance to her office is a colorful display of paints and art supplies, which she often uses to put her younger patients at ease.7 September 2022 - Aseel stands at the door with a warm and reassuring smile as patients nervously enter her office. “Anyone who’s coming to see me is not in a happy place. It’s my job to find out what is distressing them and provide support in overcoming any mental health challenges they might be facing because of their situation or life experiences,” says Aseel.
Aseel stands at the door of her office to welcome patients as they walk in. The entrance to her office is a colorful display of paints and art supplies, which she often uses to put her younger patients at ease.7 September 2022 - Aseel stands at the door with a warm and reassuring smile as patients nervously enter her office. “Anyone who’s coming to see me is not in a happy place. It’s my job to find out what is distressing them and provide support in overcoming any mental health challenges they might be facing because of their situation or life experiences,” says Aseel.
Aseel is a psychosocial counselor at the UNRWA Hebron Health Centre, providing mental health services to Palestinians living in Hebron city in the southern West Bank. The health centre covers the H2 area, which has witnessed multiple cycles of violence due to settlement activities. Many of Aseel’s patients suffer from psychological distress and mental health issues caused by the conflict and living in a constantly tense environment.
 Aseel points towards the H2 area, which has seen multiple cycles of violence due to settlement activities. Residents of the H2 area often suffer from mental health issues caused by conflict and difficult life conditions. COVID-19 has further exacerbated the situation and contributed to an increase in gender-based violence (GBV), which has enhanced the vulnerability of women and girls, Aseel explains.
Aseel points towards the H2 area, which has seen multiple cycles of violence due to settlement activities. Residents of the H2 area often suffer from mental health issues caused by conflict and difficult life conditions. COVID-19 has further exacerbated the situation and contributed to an increase in gender-based violence (GBV), which has enhanced the vulnerability of women and girls, Aseel explains.
In the last two years, Aseel has received an increased number of female patients who have developed acute stress and mental health issues as a direct consequence of experiencing violence and abuse at home. “It’s appalling and heart-breaking that women are bearing the brunt of the rising uncertainty that many families are facing due to COVID-19,” Aseel laments.
Flipping through her files, she recounts a recent case.
Salma , a young mother of two, was being verbally and physically abused by her husband after he lost his job during the peak of the COVID-19 pandemic.
She was an easy target for him. He took all his anger out on her. So much so that she started to believe that she was the cause of all his problems and would take her frustration out by beating her children. She developed severe anxiety and her mental health was spiraling,” Aseel recounts.
Salma, who lived close to the clinic eventually turned to Aseel for help. “We had four sessions, each better than the last,” Aseel explains.
“I supported her in developing mechanisms for getting her mental health under control and understanding that she is not alone. Her mindset gradually started to improve. Luckily, her husband also realized the impact his actions were having on her and that drastically changed the situation for the better.”
Unfortunately, meeting GBV survivors experiencing similar situations has become all too familiar for Aseel. But she explains that not all cases are as straightforward or have as quick a resolution as Salma’s. Some patients don’t feel confident or are trapped in circumstances where it’s extremely hard for them to reach out for support.
Women’s mental health issues can sometimes be an indicator of the GBV they are experiencing.
Often GBV survivors seeking health care at clinics are unable to be upfront about their situation due to fear and stigma. At times they don’t even recognize that they are developing mental health issues because of what they might be going through, she says.
 WHO, with support from the Big Heart Foundation, organized training to support the integration of the response to GBV into mental health and primary health care services.In the absence of adequate training, GBV and mental health cases can go undetected by primary health workers who are often the main point of contact at health facilities. Recent training provided by WHO, with support from The Big Heart Foundation, aims to address this gap.
WHO, with support from the Big Heart Foundation, organized training to support the integration of the response to GBV into mental health and primary health care services.In the absence of adequate training, GBV and mental health cases can go undetected by primary health workers who are often the main point of contact at health facilities. Recent training provided by WHO, with support from The Big Heart Foundation, aims to address this gap.
Aseel was one of 50 mental health professionals, doctors and nurses trained on the Mental Health Gap Action Programme (mhGAP) Intervention Guide (2.0), with a specific focus on screening and detecting GBV and responding to its mental health consequences.
The Guide is a crucial tool in the package of support provided by WHO since 2010 to strengthen mental health services across the occupied Palestinian territory. It is helping to expand mental health services and make them more accessible through training health workers in non-specialized health care settings and mental health professionals based at critical locations in the West Bank and Gaza. The approach aims to bridge the shortage of mental health services by ensuring that people don’t need to rely solely on specialists to access the services they need.
“The latest training of trainers, supported by The Big Heart Foundation, takes our work a step further. It aims to integrate the response to GBV in mental health and primary health care services so that GBV survivors can be screened, provided mental health support by health workers trained on the mhGAP Intervention Guide and, if needed, referred to protection and specialized rehabilitation services,” says Rajiah Abu Sway, WHO Mental Health Officer in the occupied Palestinian territory.
Plans to “cascade” the training to make it accessible to more health workers are being developed by WHO, in collaboration with the Ministry of Health.
“I’m looking forward to sharing my learning with others in my health centre. I don’t want anyone to suffer or feel that they have no one to turn to. I want to keep their hope of a better future alive,” Aseel says.
It is my duty as a health worker to ensure that I go above and beyond to help my patients, especially in Hebron, where people have already suffered a lot.


