The Gaza trauma response: WHO conducted a one-year analysis of trauma injuries in Gaza
 29 May 2019 - The World Health Organization (WHO) in collaboration with over 20 agencies conducted a detailed analysis of one year of trauma injuries in Gaza and its humanitarian impact. From 30th March 2018 to 30th March 2019, 277 Palestinians were killed and 28,014 injured.
29 May 2019 - The World Health Organization (WHO) in collaboration with over 20 agencies conducted a detailed analysis of one year of trauma injuries in Gaza and its humanitarian impact. From 30th March 2018 to 30th March 2019, 277 Palestinians were killed and 28,014 injured.
Although any health system in the world would be overwhelmed if it had to manage such a high influx of trauma casualties, the most pressing concern is the staggering number of gunshot wounds – 6872 or 25% of the total casualty caseload. Out of those, 87% were to the limbs.
172 people became permanently disabled because of their injuries, of whom 36 are children. The biggest cause of permanent disability is amputation. In one year, 121 amputations took place. WHO estimates that the damage caused by high-energy gunshot wounds has resulted in some 1209 to 1746 patients who will need specialized tertiary treatment. Without this treatment being made available in Gaza, the number of amputations may drastically increase in 2019.
“Making the services available by setting up treatment centres, such as the osteomyelitis treatment centre, deploying emergency medical teams from abroad, and providing essential medical resources, must remain a priority. But this can only be achieved with the support of the international community. Humanitarian and development actors must work side-by-side for the next phase of this response,” says Mr. Jamie McGoldrick, the Humanitarian Coordinator for the occupied Palestinian territory.
 Photo credit: WHOWHO supported the Ministry of Health and Palestine Red Crescent Society in establishing trauma stabilization points (TSPs) where wounded patients receive life-saving care close to the point of injury. TSPs have proven to save lives and also removed a burden of 41% of the trauma caseload from the already overwhelmed hospitals. Overall, it is estimated that between 435 and 1227 lives were saved thanks to the established trauma referral pathway.
Photo credit: WHOWHO supported the Ministry of Health and Palestine Red Crescent Society in establishing trauma stabilization points (TSPs) where wounded patients receive life-saving care close to the point of injury. TSPs have proven to save lives and also removed a burden of 41% of the trauma caseload from the already overwhelmed hospitals. Overall, it is estimated that between 435 and 1227 lives were saved thanks to the established trauma referral pathway.
“Trauma interventions in Gaza are not only a response to the emergency but also a longer-term investment in building the capacity of the health system to address the critical service gaps that have persisted for years,” says Dr Gerald Rockenschaub, head of WHO’s office for the occupied Palestinian territory.
The Gaza trauma response demonstrates that collective efforts, with adapted and localised solutions can provide many people with timely, life-saving care. WHO continues to support the Ministry of Health and partners in delivering critically-needed medicines and medical equipment, upgrading the trauma pathway, building capacity for health workers to respond to the growing health needs and to reinforce the quality of trauma care in Gaza.
Full report: Emergency Trauma Response to the Gaza Mass Demonstrations 2018-2019
Overcoming barriers to health care access in the West Bank with mobile clinics
 Women from Zakariah village. Credit:WHO27 May 2019 - A small room in an improvised school in Zakariah village, the West Bank, occupied Palestinian territory, used to serve as a patient consultation space for a mobile clinic providing primary healthcare services in the area. Last year, the clinic stopped operating due to a lack of funding, leaving a community of 650 without access to essential health care.
Women from Zakariah village. Credit:WHO27 May 2019 - A small room in an improvised school in Zakariah village, the West Bank, occupied Palestinian territory, used to serve as a patient consultation space for a mobile clinic providing primary healthcare services in the area. Last year, the clinic stopped operating due to a lack of funding, leaving a community of 650 without access to essential health care.
Since then, to get even basic health services, Zakariah residents have to travel to a health clinic in Bethlehem – about 12 kilometres from the village. The distance, however, is not the biggest barrier for the community to access the health care they need. A journey to the town is costly, time-consuming and frequently stressful. The villagers need to pass through a number of checkpoints which makes access often unpredictable and at times heavily restricted. Zakariah is surrounded by settlements that hamper free movement for the community. It is not safe for residents to leave the village on foot, meaning that they need a car to reach Bethlehem. The majority does not have a car and there is no public transport, so many in the community rely on the only taxi driver in the village to reach health facilities for appointments.
“It’s very hard for the villagers to see a doctor,” says Zakariah’s community leader. He is the first person people come to in cases of emergency. “When there is a case that requires urgent medical attention, I am looking for ways to either reach the hospital in Bethlehem or bring an ambulance to the village, but these trips can sometimes take hours.” But in emergency situations, any delay in care can have serious adverse consequences on patient outcomes. A woman from the community took first aid training from the mobile team to ensure immediate assistance is available. She can also provide non-prescription medication to reduce fever and pain as a temporary measure.
Zakariah village is among 100 communities or so with about 114,000 residents in Area C* that have limited or no access to primary healthcare services. The geographical, legal and administrative fragmentation of the West Bank creates barriers for them to access health, but these obstacles are particularly severe for those in Area C. Like in Zakariah, many communities rely on mobile health clinics to get primary health care.
A team of two general practitioners, a women’s health specialist and a nurse used to visit Zakariah village twice a month offering free consultations, medication and providing basic health services such as screening for noncommunicable diseases, immunization, women health services, lab analysis and health education.
 A room that used to serve as a patient consultation space for a mobile clinic providing primary healthcare services. Credit:WHONow, people from the village only go to the hospital when there is an urgent need, such as for childbirth or in the case of injury. This situation can be particularly worrisome for the elderly, who make up much of Zakariah’s community, with hypertension, diabetes and other chronic diseases that require regular checkups, medical attention and daily medication.
A room that used to serve as a patient consultation space for a mobile clinic providing primary healthcare services. Credit:WHONow, people from the village only go to the hospital when there is an urgent need, such as for childbirth or in the case of injury. This situation can be particularly worrisome for the elderly, who make up much of Zakariah’s community, with hypertension, diabetes and other chronic diseases that require regular checkups, medical attention and daily medication.
“My husband died from kidney failure, and I have diabetes and blood pressure,” says Hajra, a 65-year-old woman from the community. “I have to pay for medicine from my pocket, and it’s often half of my monthly income.”Many of Hajra’s neighbours cannot afford medicine at all.
Mobile clinics offer viable options to improve access to primary health care for such vulnerable and remote populations. Currently, the Palestinian Ministry of Health and health partners are reaching around 140,000 people in Area C, the West Bank. To deliver health care to underserved areas, the World Health Organization with its partner CARE International supports the provision of quality primary healthcare services through mobile clinics to about a further 12,000 people in 19 vulnerable communities in Hebron, Bethlehem and the North Jordan Valley areas. In addition to essential health services, the teams will also be providing psychosocial support to the populations. This project is possible thanks to the contribution from the UN Central Emergency Response Fund.
A director of Zakariah’s school said the mobile clinic services went beyond health care and had an overall positive impact on the community: “They were bringing a feeling of safety and normality to our people devastated by a lack of security, movement restriction, constant pressure and stress.”
*Over 60% of the West Bank is considered Area C, where Israel retains near exclusive control, including over law enforcement, planning and construction.
Health attacks continue during Gaza’s Great March of Return
 Mohamed Abu Taema. Credit: WHO20 May 2019 – Mohamed, a 24-year-old first responder, was injured during demonstrations in Khan Younis, Gaza, on Friday 10 March. He had seen a child of approximately 12 years injured from gas inhalation near the Gaza fence, and had gone forward to treat him and bring him to the nearby medical point of the Ministry of Health:
Mohamed Abu Taema. Credit: WHO20 May 2019 – Mohamed, a 24-year-old first responder, was injured during demonstrations in Khan Younis, Gaza, on Friday 10 March. He had seen a child of approximately 12 years injured from gas inhalation near the Gaza fence, and had gone forward to treat him and bring him to the nearby medical point of the Ministry of Health:
“I went forward and carried him back [away from the Gaza fence]. Then I stopped at a distance of 150 metres with my colleague to provide first aid to the child. After we had finished, I stood and was hit by a gas canister on the left side my forehead. They took me to the medical point and then transferred me by ambulance to the European Gaza Hospital. I lost consciousness in the ambulance on the way to hospital.”
He sustained a fracture and bleeding into his skull, needing 5 stitches in his head and admission to hospital for investigations and observation.
Mohamed is one of 35 first responders volunteering with Watan medical team. The team was established at the start of the Great March of Return demonstrations on 30 March 2018. Mohamed joined the team in August 2018, after an intensive course on the provision of first aid in the field.
WHO met Mohamed on Monday 13 May, when he was being discharged from the European Gaza Hospital. His colleagues from Watan team had come to help him. Gaza volunteers work at great personal risk to treat injured persons. Since demonstrations as part of Gaza’s Great March of Return began on 30 March 2018, until the end of April 2019, 3 health workers have been killed and 745 injured in 462 recorded incidents against health staff and facilities.
This is Mohamed’s fourth injury from a gas canister since he began work with Watan team. He also sustained countless injuries from gas inhalation, including one occasion where he lost consciousness and was taken to hospital as a result of gas inhalation. Mohamed’s colleagues, too, discussed the extent of injuries they sustained during protests and their frustration that violence towards them continues. The leader of Mohamed’s field team showed a scar on his chest from a previous gas canister injury. He reported that this injury was one of several injuries he had sustained and not reported.
Mohamed lives in area of Khan Younis with his wife, 7-month-old boy and extended family. Like almost three quarters of young people in Gaza, Mohamed has been unable to find work. He studied psychology for one year, but he had to stop when he could no longer afford the fees or transportation to reach his university.
“This work, I love it. Through this work, I’m helping the people of my nation. I have one goal, even when I’m injured – giving first aid assistance to others helps me to recover. That’s the most important thing. If the whole world thought like me, no one would be left injured! Beyond going [to the demonstrations] as a paramedic, I go normally – like all people. I’ve been discharged from the hospital, but on Wednesday [15 May] I’m going to the field… I dream of return, like all Palestinians.”
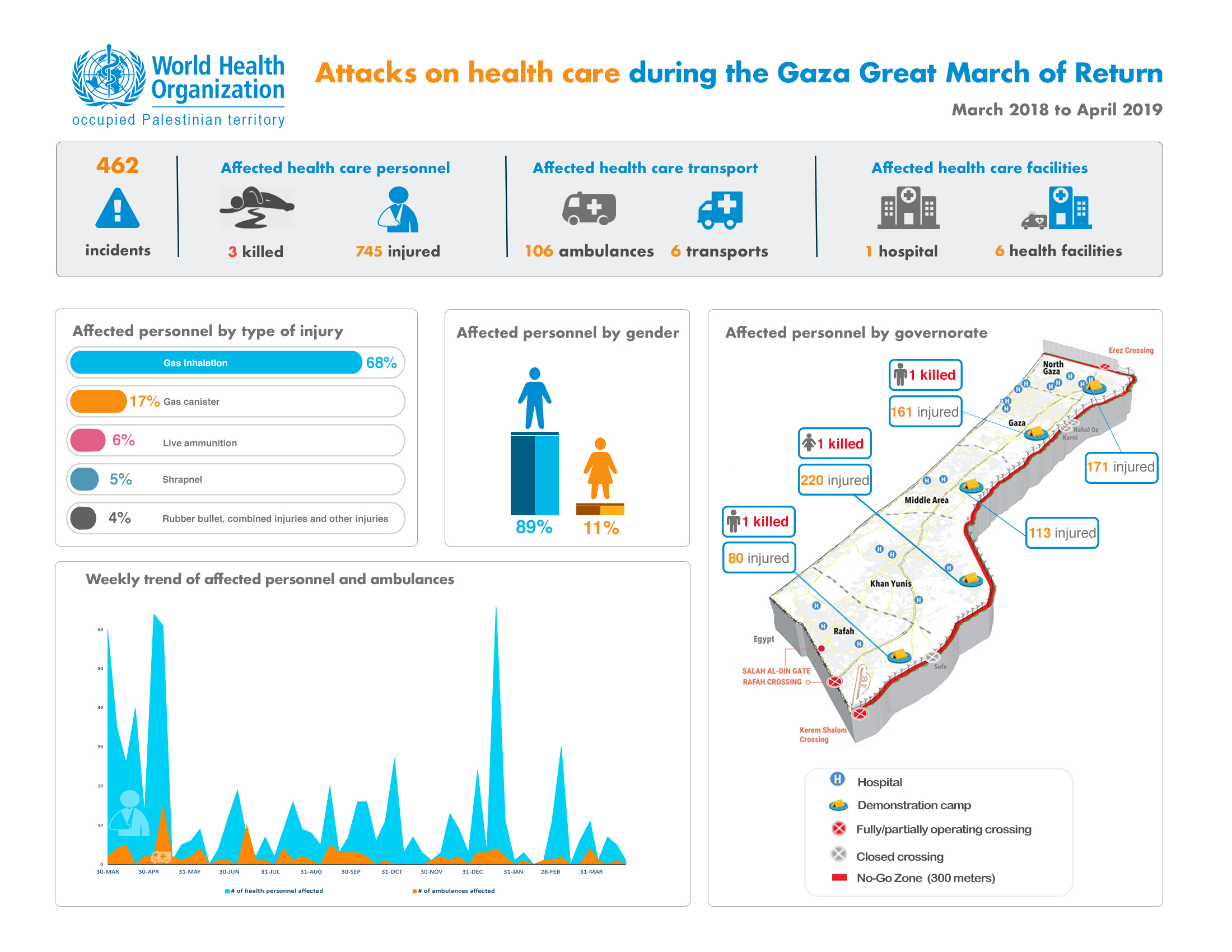
Attacks on health care during the Gaza Great March of Return
UN Special Coordinator visited WHO solar electrification project in Gaza
 Nickolay Mladenov visiting solar plant at Nasser hospital in Gaza15 May 2019, Gaza - UN Special Coordinator for the Middle East Peace Process Nickolay Mladenov visited a solar electrification project at Nasser hospital in Khan Yunis, Gaza. The project is implemented by the World Health Organization (WHO) with financial support from the Government of Japan. It aims to contribute to the continuous functioning and resilience of the hospital by equipping it with solar panels as an alternative source of electricity.
Nickolay Mladenov visiting solar plant at Nasser hospital in Gaza15 May 2019, Gaza - UN Special Coordinator for the Middle East Peace Process Nickolay Mladenov visited a solar electrification project at Nasser hospital in Khan Yunis, Gaza. The project is implemented by the World Health Organization (WHO) with financial support from the Government of Japan. It aims to contribute to the continuous functioning and resilience of the hospital by equipping it with solar panels as an alternative source of electricity.
Gaza has been affected by protracted electricity shortages for over a decade. As a result, the health sector relies on donated fuel to run back-up generators in health facilities to sustain critical services when electricity is unavailable from the mains grid supply. The solar electrification project will reduce the health sector’s dependency on emergency fuel and, therefore, the impact of the electricity crisis on patients.
The official opening of the solar plant and the project handover ceremony between The Government of Japan, WHO and the Ministry of Health will take place in June 2019.


